Missouri S&T biosciences fighting COVID-19
Posted by Sarah Potter

Phelps Health workers at a COVID-19 testing site in Rolla, Missouri. Photo by Tom Wagner/Missouri S&T
Missouri S&T students who studied biosciences have been on the front lines fighting the COVID-19 pandemic in the last year and others are seeing secondary patient effects every day in their health care fields. They discuss some of the toughest and most rewarding parts of their jobs and offer their best advice for the public.
- Claire Brewer, BSci’17, works on the front lines of the COVID-19 fight as a paramedic for Abbott EMS in St. Louis.
- Dr. Taylor Hahn, BSci’09, has worked as an active duty OB/GYN in the U.S. Air Force and now works as a civilian OB/GYN in Indianapolis.
- Toni Knar, BSci’14, is a hospitalist physician assistant (PA) working at Bellin Health in Green Bay, Wisconsin.
- Justin Lovelady, BSci’14, has a bachelor’s of science in nursing (BSN) degree and is a travel registered nurse (RN) who has worked in Connecticut and Georgia fighting COVID-19. He lives in St. Louis.
- Dr. Megan Ottomeyer, BSci’12, MS BSci’13, works in the neonatal intensive care unit at SSM Health Cardinal Glennon Children’s Hospital in St. Louis as a neonatal-perinatal medicine fellow physician.
- Kiran Patel, BSci’15, is a physician assistant (PA) currently administering the COVID-19 vaccine in Junction City, Kansas.
What has been the toughest part of your job?

Claire Brewer: In April 2020, I flew to New York City on a FEMA deployment and worked 18 days in a row with shifts lasting anywhere from 12 to 16 hours. Hospitals were full, FDNY (the New York City Fire Department) had many employees either sick with COVID-19 or deceased from it, and every call was straining on us physically, emotionally and mentally. It was so frustrating because we as first responders could only manage the symptoms and get patients to the hospital, and on some calls, I almost felt like I wasn’t doing enough to help them. But I am forever grateful that I was able to do my part and help my fellow EMS family. If I never have to go back to NYC for work, then I’ll be happy.
Dr. Taylor Hahn: The toughest part is trying to keep patients safe and protected during this pandemic while much of our evidence for care related to COVID-19 has been developing in real time. In particular, caring for pregnant women with COVID-19 who are very scared not only for themselves, but also their babies, has been mentally and emotionally challenging and straining.
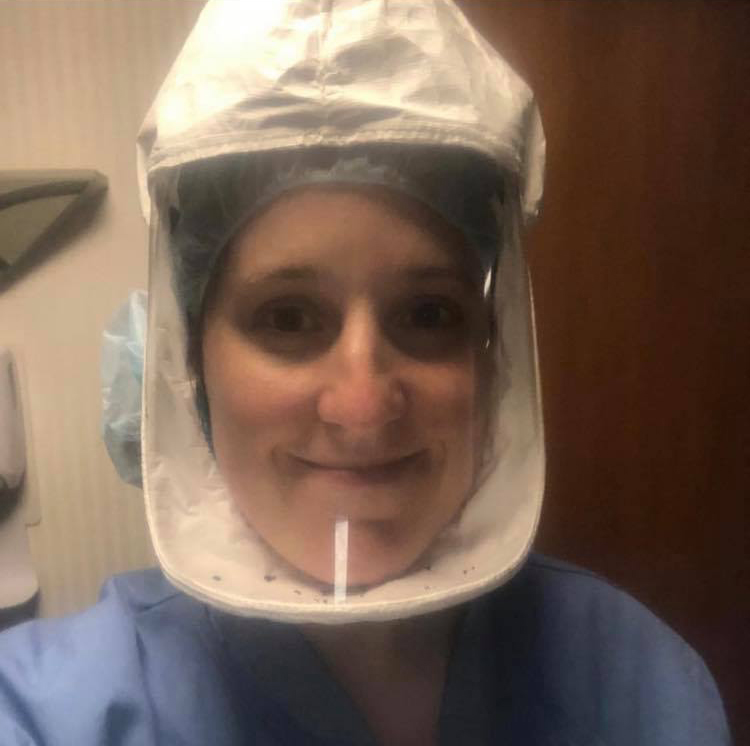
Toni Knar: In our community, a lot of the meat factories were hit the hardest. These factories were labeled essential, and a large number of employees continued to show up for work. The employees were near one another and unaware of the common signs and symptoms of the COVID-19 virus. In the beginning, there was not a lot of outreach in the community about educating high-risk workers on these matters.
After we saw how this virus was affecting the meat factory employees, Bellin Health gathered volunteers to travel to these sites, perform screenings on employees for signs/symptoms of COVID-19 virus, perform testing with nasal swabs and establish follow-up with a provider. Bellin Health established respiratory clinics that were a source of information to the public about the COVID-19 virus.
Dr. Megan Ottomeyer: The toughest part was one particular experience I had with a very sick baby with a COVID-positive parent. The baby was dying, and the parent had elected to redirect care toward comfort measures, however, the parent also became severely symptomatic and tested positive for COVID. It became very difficult to balance providing end-of-life palliative care, allowing the parent to have those precious moments holding the baby at the end of his life, and protecting the other patients, families and staff in the NICU from exposure to this symptomatic parent. These types of situations are ethically taxing, emotionally draining, and just plain hard. That’s why it’s so disheartening then when people either don’t take COVID-19 seriously or don’t do their part to ameliorate the risks.

Justin Lovelady: Pointing out the toughest part of a nurse’s job is a loaded question. The brutal truth is that the toughest part of my job is death. Day in and day out you try your hardest to prevent the worst. You clock in, watch humans suffer and be separated from their families (since others were not allowed to visit due to the virus), and all you can do is your best, utilizing your skills and knowledge to the fullest and try to go above and beyond to make people as comfortable as possible.
Kiran Patel: One of the toughest parts during the pandemic has been treating patients who are very ill because of this virus and have no family members by their side due to the restrictions that have been set. Also, many eligible vaccine recipients are refusing due to skepticism of the vaccine. However, studies have shown the efficacy of this vaccine, and I highly encourage everyone to do their part and help protect their friends and family.
What has been the most rewarding part of the job?
Brewer: I have been fortunate enough to work shifts giving the Pfizer vaccine with the St. Louis County Department of Public Health on my off days. It has been so rewarding to be able to give something that can help save so many lives! After working in NYC and not feeling like I was able to do much for my patients, this has been a wonderful opportunity for me as a healthcare provider!

Hahn: Continuing to bring new life into the world and see the joy and hope in the eyes of mothers and fathers despite the persistent worry of COVID-19 transmission. Being able to offer lifesaving and life-changing surgery to strong, resilient women who often put the health of their families ahead of their own.
Knar: By far, the most rewarding part of the job was seeing patients that were placed on additional supplemental oxygen like a nasal cannula, BiPAP, and ventilator, weaned off to room air and be discharged home.

Ottomeyer: The most rewarding part has been seeing scientists share data for the common good. Worldwide there’s been an inspiring amount of collaboration, and it’s really admirable. It’s also been nice to see how some folks have really stepped up to support local businesses, hospitals, clinics and just their communities in general to help get all of us through this pandemic.
Lovelady: The most rewarding part of all this is getting to discharge a COVID recovered patient and getting to meet and work with amazing people from all over. While in Connecticut, the hospital I was at would announce over the intercom the discharge of COVID recovered patient. It gave everyone hope – the patients and the workforce. At my current hospital, we are seeing a significant decrease in COVID cases. Being able to watch those numbers of patients drop is outstanding.
Patel: I became a PA to serve the community and provide quality healthcare to my patients. Going through school with this pandemic immediately called for students still in training to do their part. This will be something that I will talk about for a very long time. It is an honor and privilege to be able to do what I do, and I hope to continue to grow and learn in my role in the health care world.
What advice would you give the public about fighting COVID-19?
Brewer: Trust science. Wear your mask. Wash your hands. Socially distance. But most importantly, get vaccinated as soon as you can. I am so thankful that I received the Pfizer vaccination and am better protected for myself, my significant other, and every patient I interact with.
Hahn: Seek out medical professionals and non-biased evidence about the virus and the pandemic and communicate your concerns with your doctor. There is so much sensationalized and inaccurate information on the internet and through social media. We’re all in this together, and our goals as physicians are the same as yours – to prevent the spread of this virus and protect your health and the health of your family and friends.
Knar: First, follow the basic steps to help prevent the spread of COVID-19: hand hygiene, masking up, quarantining with signs or symptoms of the COVID-19 virus, and quarantining after exposure to someone who has tested positive have been instrumental in fighting the COVID-19 virus. Second, knowledge is power. The CDC, PubMed, and Medscape are three of the many resources on this subject that are accepted by the medical community. Your primary care providers are a wealth of knowledge, and my advice is to talk with them about what sites can be trusted. Third, have a discussion rather than a one-sided argument and know the difference between the two. With social media, try to avoid being reactive and accusatory when jumping into these subjects. Choose to move forward with grace; broaden your perspective by trying to understand why a certain someone is using a certain news source; and make it a goal to have a civil discussion with those in your community.
Ottomeyer: My advice would be to listen to the experts. There’s a crazy amount of misinformation out there and an even crazier amount of people who willingly buy into it. Use reliable sources, check the facts, and just use common sense. Also, be kind to one another. This past year wasn’t the one that anyone had planned. We all want to get back to something close to our normal, pre-COVID lives. This is a global crisis, and that means we need to support each other and care for each other’s wellbeing more than ever.
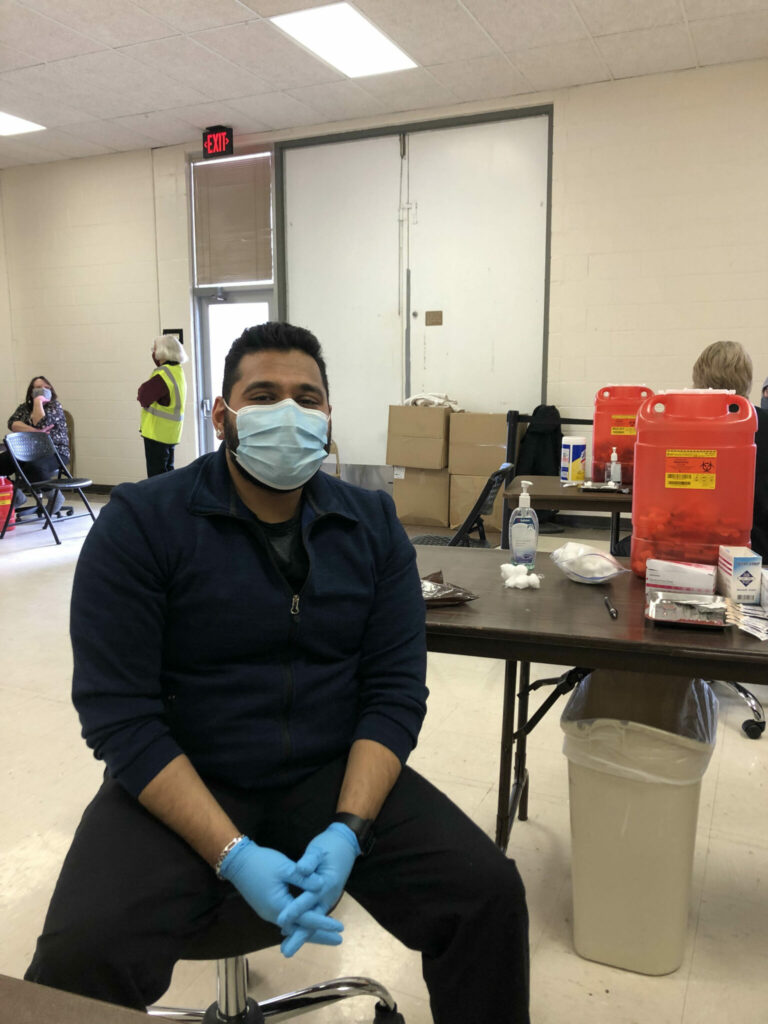
Lovelady: Fighting ignorance is the most challenging part of this whole situation. COVID-19 is real. The death toll is real. The psychological and physical stress is real. The exhaustion of healthcare workers is real. It really is simple … wear your mask (yes, over your nose, too), distance yourself, avoid crowds, stay home if you are sick, utilize all those contactless options available, get vaccinated if you can, and, please, WASH YOUR HANDS.
Patel: The best advice I would give is to respect and adhere to the restrictions that have been set to fight this pandemic. Avoid close contact and unnecessary travel, and get the vaccine. Remember that this is not for just you but for the friends, family and community that you love.
I greatly appreciate all the ‘spot-on’ advice on COVID-19 from the BioSci alumni in the health fields. Thank you for speaking out. I hope you are heard!