Health care teams respond to COVID-19
Posted by Delia Croessmann
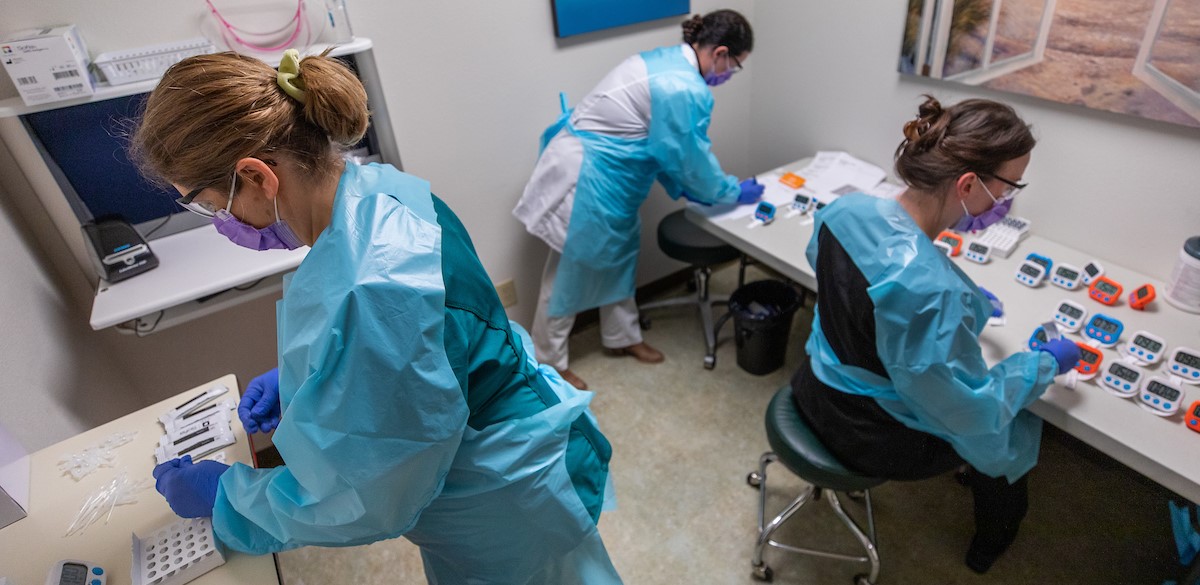
From left, Tracy Fair-Parsons, physician’s assistant, Mindy Bryson, nurse practitioner, and Marisa Yates, physician’s assistant, perform a COVID-19 group test in a sequence that produces a result every 11 seconds. They quickly process COVID-19 tests from members of high-contact sports teams who are checked every two weeks. With this system, they can process up to 40 tests an hour. Photo by Andrew Layton.
With no known cases of COVID-19 on campus at the time, Missouri S&T’s 2020 cancellation of its iconic St. Pat’s celebration seemed extreme to some, but that March 11 announcement occurred on the same day the World Health Organization declared the coronavirus a global pandemic.
And only two days later, S&T announced it would send students home to finish the spring semester online.
Keeping campus safe while providing an on-campus, academic living experience was—and still is—the objective of S&T’s 32-member Incident Command Team, which was formed to manage the changes the pandemic required of the university, says Dr. Dennis Goodman, S&T’s director of student health and chief medical officer.
“The virus is still not well understood,” says Goodman. “We are learning more every day and must adapt our response to the developing science.”
The rapid-response decisions the virus brings to campus drive the day-in, day-out work of S&T’s campus COVID-19 response team of contact tracers, testing coordinators and care managers that operate from S&T’s Student Health Services (SHS). The combined efforts of these teams, students and the entire campus community have helped maintain a relatively low and manageable rate of confirmed cases at S&T since the fall semester began Aug. 24. As of November 10, out of 6,760 students on campus, 173 have tested positive and only 34 out of 1,256 employees. Almost all have recovered.
But these encouraging results have demanded many additional hours of work from the SHS team, as well as relentless vigilance to the current guidance of the Centers for Disease Control and Prevention (CDC), the American College Health Association, Missouri state briefings and various global health initiatives. All of this comes in addition to the staff’s responsibility to provide the same level of care as it did before COVID-19 arrived.
Stopping the spread, strategically
The ICT’s six-phase repopulation plan sent faculty, staff and students home in March and gradually brought them back in segments until the fall semester started. It curbed the spread of COVID-19, especially by requiring students to quarantine on campus two weeks before classes started.
“S&T’s traditional ‘O’ (orientation) week became ‘Q’ (quarantine) week, but it worked,” says Mindy Bryson, S&T’s director of student health operations and family nurse practitioner.

Mindy Bryson, S&T’s director of student health operations and family nurse practitioner, programs the Sofia 2 analyzer to read a COVID-19 test. Photo by Andrew Layton.
Goodman says they learned a lesson from Michigan State University and the University of Notre Dame, two Midwestern schools that had to shut down their campuses only eight days after school started. Michigan State went fully remote for the semester, and Notre Dame moved its undergraduate instruction online for two weeks.
“They tested all their students before they came to campus, and it may have created a false sense of security,” says Goodman, who consulted with both universities. “A better approach may be an ongoing daily evaluation of the campus community with emphasis on facial coverings, social distancing, limiting gatherings, and prompt contact tracing with resulting quarantine and isolation.”
“If you test positive for COVID-19 while in quarantine, you have no contacts,” Bryson adds. “That is the key to stopping the spread.”
Improved testing

Fortunately, in-office rapid antigen testing is now the norm at S&T. The test system SHS obtained in August produces single or multiple test results within 15 minutes. For large groups such as athletic teams, SHS can run up to 40 tests an hour. Bryson says this is a vast improvement over a process that has progressed from sending the tests to the CDC in early spring, then to the state of Missouri, and then to Phelps Health, all of which required days of waiting for results and delayed contact tracing.
Front line contact tracing
Contact tracing lets people know they may have been exposed to COVID-19 and should monitor their health for symptoms. Goodman says the SHS contact tracers worked many 18-hour days through surges of COVID-19 cases in the summer until he was able to enlist S&T’s athletic trainers to help when they returned to reduced sports activities in the fall. Regardless, the entire SHS team still works from 7 a.m. to 5 p.m. most days, handling the everyday health problems students present in addition to the COVID-19 work.
“If a student tests positive at 5 p.m. and has 20 contacts, our contact tracers must start the work then and continue until the job is done,” says Bryson. “Their day is not over until all the contacts have been identified and their quarantine arrangements are made. That includes getting them their own room and bathroom, if possible, and making alternative arrangements for their classes, meals, laundry and excuses from work.”
To monitor the behaviors of the quarantined contacts, the SHS now relies on Sara Alert, an open source technology tool that automates the process of monitoring and reporting of individuals exposed to or infected with COVID-19. Sara Alert can retain data and send messages to up to 400 people in quarantine, an exponential task that team members review every day.
Success and responsibility
Goodman says one of the major successes of S&T’s COVID-19 management is that the virus hasn’t spread in the classrooms. “It is difficult to modify classes,” says Goodman. “Only 30% of students can attend in person, making it necessary to construct hybrid and online classes.”
He gives credit to the collaborative support of Dr. Stephen Roberts, interim provost and executive vice chancellor of academic affairs, the university’s learning transition team, the facility operations staff’s implementation of safe practices, and the information technology department’s implementation of classroom technology.
Bryson’s biggest concern at this point is COVID-19 fatigue — for her staff, the students, university employees and the country altogether.
“In the medical community, we see people who are tired of taking precautions, and the infection rate is increasing, and hospitals are getting crowded,” she says. “It’s hard for people to recognize that when they feel in a safe bubble on our campus.
“Our students have been so good to this point — they’ve literally stopped the spread, and now we have to keep all this going.”
Goodman says managing COVID-19 on campus is lot of responsibility.
“I had training in the military in epidemiology and infection control, but am now in a role to keep over 8,000 people safe,” says Goodman.
STOP THE SPREAD
S&T’s Student Health Services staff advises campus community members to remain vigilant in stopping the spread of COVID-19, especially as they make plans for the holidays:
- Perform a health check before coming to campus. If you feel sick, do not come.
- Continue to wear face coverings in accordance with S&T’s updated policy for students, faculty, staff and visitors.
- Maintain physical distancing of six feet between individuals on and off campus.
- Wash your hands frequently for 20 seconds or use an alcohol-based hand sanitizer.
- Avoid touching your eyes, nose and mouth.
- Cough into your elbow of tissue. Dispose of tissue and wash your hands.
Congratulations to all at MO S&T for keeping COVID-19 mostly at bay.
The holidays and other transitions pose a new issue to face- but with potential good news about
the mRNA type vaccines that may be very effective.
That means, of course, that extensive planning and execution for vaccinations in the next few months
must begin now (and I am sure that the team is feverishly doing so).
MO S&T is proving our greatness each and every day!
Congratulations! I have been impressed as a parent of a student. Has the university published recommendations for the Thanksgiving break?
Hi Karen,
Thank you for contacting us. Here are S&T’s travel guidelines for Thanksgiving: https://econnection.mst.edu/2020/11/message-from-chief-medical-officer-thanksgiving-safety-and-safe-return-to-campus/. Within this article, there are several links that give very specific guidance.
Best regards,
Delia Croessmann